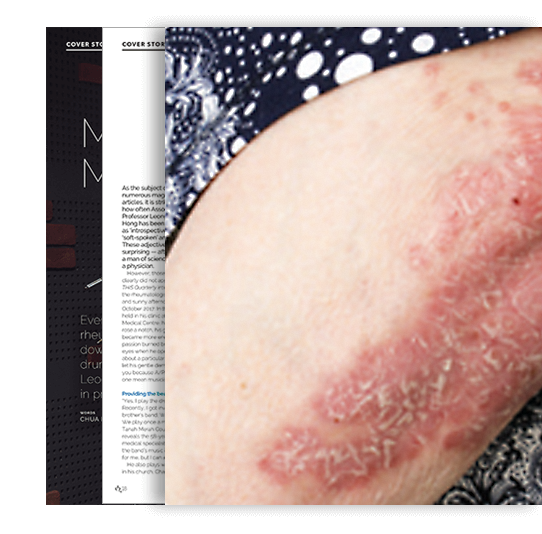
Psoriatic Arthritis:
Inflamed Skin
and Joints
2017
Peolple with this condition suffer the double whammyof having symptoms in both the skin nd joints.
According to the Centers for Disease Control and Prevention in the US, more than one-third of adults who have arthritis complain that their condition interferes with work and leisure activities. Up to 25% of them also reveal that it is a big source of pain, giving it a score of seven or higher on a 10-point scale.
Inflammatory arthritis refers to the inflammation of one or more of your joints. The most obvious symptoms are pain, swelling and morning stiffness in the affected joints.
Arthritis exists in myriad forms - there are more than 100 types of arthritis and related diseases. The most common ones include rheumatoid arthritis, osteoarthritis, gout, fibromyalgia and psoriatic arthritis. All of them cause pain in different ways. This article focuses on the condition known as psoriatic arthritis (PsA).
